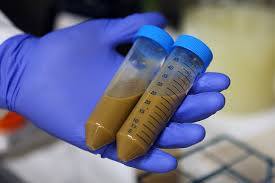
Almost 50% of the patients in the examination revealed huge improvement in their manifestations in the wake of getting a fecal transplant.
Fecal transplants may facilitate the difficult and troubling indications of touchy gut disorder — if those transplants originate from individuals named “super donors,” as per an investigation introduced Sunday.
The huge, randomized twofold visually impaired fake treatment controlled preliminary — thought about the highest quality level for therapeutic research — found that fecal microbiota transplantation essentially improved IBS manifestations in almost 50% of patients. The examination was introduced by lead specialist Magdy El-Salhy, a teacher in the branch of clinical prescription at the University of Bergen in Norway, at the yearly United European Gastroenterology Week in Spain.
An expected 10 to 15 percent of Americans have IBS, as indicated by the American College of Gastroenterology. Indications can incorporate stomach cramping and swelling just as obstruction and looseness of the bowels. In spite of the fact that the condition can cause huge torment and distress, it doesn’t bring about harm to the digestion tracts.
The reason for IBS is obscure, however a few specialists have proposed that it may be connected to variations from the norm in the microbiome, the plenty of microorganisms that populate the gut.
Fecal transplants, or fecal microbiota transplantation (FMT), work by repopulating the gut with a more advantageous cluster of microorganisms. Stool from a giver is handled and after that transplanted into the gut of the beneficiary.
To investigate whether FMT could quiet IBS side effects, El-Salhy and their partners enrolled 164 patients who had been determined to have the condition and who experienced moderate to extreme indications.

Before treatment the patients were gotten some information about their side effects. They were then haphazardly doled out to get 30 grams of an answer containing their very own defecation — the fake treatment — or one of two dosages (30g or 60g) containing excrement from an alleged super benefactor. The portions were conveyed to the small digestive system through a cylinder embedded into the mouth and down the throat.
A quarter of a year later, the patients were again approached to detail their side effects. Contrasted with before treatment, 23.6 percent of patients in the fake treatment gathering revealed moderate manifestation improvement. In the gathering that got the lower portion of super contributor excrement, 76.9 detailed a moderate reaction, and in the higher portion gathering, 89.1 percent.
Progressively significant, they additionally discovered side effect abatement — implying that indications left totally — in 35.2 percent of those in the lower portion gathering, and in 47.3 percent of those in the higher portion gathering. That is contrasted with 5.5 percent of the patients in the fake treatment bunch who announced manifestation abatement.
After one year, El-Salhy said that the impacts seem to have kept going. “The preliminary results [suggest] most, 90 to 95 percent, of the responded patients are still well and about 50 percent are still ‘cured,’” they wrote in an email.
Past investigations have additionally taken a gander at the impacts of FMT on IBS side effects, and have discovered blended outcomes. El-Salhy credited the adequacy of the treatment given in his examination to the super contributor’s particular microbiota.
“We had a carefully selected donor from several candidates who had traits known to affect intestinal microbiota positively,” El-Salhy said. In general, the benefactor was solid, had been bosom nourished, devoured a nutritious eating regimen, took no customary meds, was a nonsmoker and had taken anti-microbials just a couple of times, they said.
Specialists were gladdened by the outcomes, however fairly doubtful about the possibility of a super benefactor, since it wasn’t clear how El-Salhy’s outcomes could be copied.
“These are very promising results that will certainly generate a lot of interest and attention because there is a great interest in these kinds of therapeutics for IBS,” said Dr. Alexander Khoruts, a teacher of medication and medicinal chief of the Microbiota Therapeutics Program at the University of Minnesota.
“But it’s not clear how you could find another ‘super donor’ to reproduce these results.”
Dr. Jonathan Jacobs, an associate teacher of medication at the University of California, Los Angeles Medical School and chief of the UCLA Microbiome Core, concurred. In the event that for reasons unknown, these sorts of results are conceivable just with stool from a super giver, who could be an irregularity, “then we wouldn’t be any better off,” they said.
Given the blended outcomes in past examinations treating IBS with FMT, “I’m not sure this study will allow us to conclude that a super donor is needed, but rather that FMT in general needs to be validated in additional studies,” said Dr. Purna Kashyap, a partner educator of medication, physiology and biomedical building and co-chief of the Microbiome Program at the Mayo Clinic.
For sure, it’s as yet indistinct what job gut microorganisms play in IBS, and truth be told, most of studies demonstrate that the microbiome of individuals with IBS is like that of sound individuals, Kashyap wrote in an email. In light of that, “how do you decide what a good donor should be?” Kashyap included.
- Effective Time Management – This article by Mr. Ben Bander Abudawood - November 6, 2021
- Craig Cavanagh, the singer and manager of major nightclub in Liverpool called Ink Bar - February 26, 2021
- How to Receive All Over Google’s New Photo Sync Limits on Android - July 1, 2020